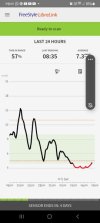
There is no wrong choice of breakfast as long as you bolus correctly for it. However I am sure I have mentioned to you before that you don't need to eat
OMG! Just the thought of not eating has sent God's fear in me. I can't seem to move away from the thought of feeling hungry, specially at night time.
breakfast if you don't want to. I sometimes head out very early on just a cup of coffee and either have brunch or lunch later in the day. The benefit of a basal/bolus insulin regime is that you can eat your meals when you like or not eat at all ie skip meals or graze all day long. You just have to inject insulin as and when you need it.
I used to be like that. Had tea and off i went to work.
I inject my bolus for breakfast plus any correction if I am above range, plus another 1.5-2 units to cover Foot on the Floor Syndrome BEFORE I get out of bed.
The range given to me is 10mmol/L. I am not happy about it but there is nothing i can do, despite all my hard efforts. How do you establish FOTF Syndrome? Do you take it every day irrespective of your readings? And correctional dose? How much are you out of range before adding extra units? What if it is a case on every morning? I ve been advised that 1u for 2 or 3mmol/L. I work it on the basis of 1:3. Not that it works anyway.
Then I visit the bathroom and make a coffee and make my breakfast and sit down to catch up with the news here on the forum whilst I wait for my insulin to kick in (usually 45 mins) and then I eat my breakfast. I scan regularly to watch for my levels starting to come down and usually mid 5s is when I eat my breakfast.
I wait for 15 to 20mins, as told. Honestly speaking, I got told off by the DSN when told her that I waited for much longer than anticipated before eating. How long do you wait for? was my next question, but you ve already answered that.
If I am not going to have any breakfast I will still inject that 1.5-2 units to cover Foot on the floor and any correction needed, but not the actual breakfast bolus.
Does that not send you in a hypo? I only did this once where I basaled and not bolused for a day and half. I ended up in the hospital with sharply rising ketones. It is called a liver dump, I was told.
i just look at my graph for my overnight basal test, in fact I just look at my graph for all my basal tests. I don't go off actual readings, I go off if my graph is drifting upwards or drifting downwards or nice and level.
I tend to avoid the graphs as they make no or very little sense to me.
I often skip meals because I don't feel the need to eat 3 meals a day,
I can eat for two, if i could. Always hungry. Even tried going to bed to distract myself. It works sometimes.
so I regularly check my basal is holding me steady at different times of the day and night without really planning a basal test as such, I just do it naturally/instinctively so it is quite hard for me to advise you on this.
Fair enough. I am sure i will reach there one day.
The general DAFNE guidance is that if you need corrections during the day 3 days in a row then you need to look at increasing your basal insulin. Then you are supposed to leave it for 3 days to assess the impact of your change before you consider changing it again. When you get it right, everything is so much less frustrating.
Yes, when one gets it right but when is that going to come my way? Re corrections - i understand the 3 days rule. What if one needs corrections more than once in a day for 3 days?
Do you only scan 8 times a day? For comparison, I average 35 scans a day over the past 30 days. All that information gives me a much better insight into what my levels are doing and whether I need to take any action or not. If I only scanned 8 times a day, I might as well just be finger pricking.
I am not making this up, the DSN ticked me off for scanning. You are constantly scanning. Then you are looking at those readings and getting yourself in a knot. Not necessary, she told me. In the days before the readers and scanners, people only checked 2 times a day and that's it.
What do you have your high and low alarms set at?
my low alarm is set at 4.5 and high at 13mmol/L.
To be honest, your graph is of much more use to you than the log as it shows all the ups and downs.
I need to learn to read the graphs correctly.
So.... the first of April one...
Am I right in thinking you went to bed on 13.3 and woke up on 16.3. What did you have for tea and what time did you eat?
I went to bed on 31st March at 12.7mmol/L. Scanned in the middle of the night and it read 13.3mmol/L. I woke up in the morning at 8:40, reading 16.3mmol/L. I basaled (14u) and bolused (9u) plus 1u as correctional dose. Breakfast usually is 32g of Carbs. Looking back it is not making sense to me either.
I was borderline hypo L2 3.9 and on GM 4.4, around 7:00pm. Pan-fried veg with salad and a pear. Total carbs 55g. Bolused 8u NR. Ratio 1:7.
Around 11:00, it read 7.7. I basaled 14u and went to sleep.
On April 2nd at midnight it read 13.0. Woke up in the morning, to 11.1. Bolused and basaled, ate breakfast around 9:00am. Went out to the Craft store. By 11:00, I was going down, 9.9mmol/L. At 2:00pm, it read 3.8 on L2 and GM read 4.2. I ate a small banana as I was heading home.
6:00pm the reading was 13.1. It continued going up. At 7:45 it went as high as 20.0mmol/L on the scanner. Then it started going down to L2 16.8 (14.8 on the GM) and then 16.0. At bed time I was 14.6. I basaled and went to bed only to be woken up reading 19.4.
Would it help if i send you the images of graphs?
If you hadn't injected any insulin in the previous 4 hours before bed, did you consider injecting a correction at bedtime to bring those levels down a bit more into range?
I would have jabbed a couple of units if there was no longer any active bolus insulin in my system. If your correction factor is 3 then that would have brought you down to about 7.3,
How do i establish what my real correction factor is? I just go with 3u per extra unit.
assuming I knew my evening basal dose was correct and holding me steady. Looking at your graph will help you to see if your basal is holding you steady, unless you ate late or your meal contained slow release foods.
You have mentioned that you have a milky drink at bedtime I think.... Do you bolus for that drink?
In that milky drink it was mere ⅓ cup of milk, less than 100ml (<4g) and the rest was water. So I did not see the need to bolus.
Am I right in thinking you woke up at 8.38am on 16.3. Did you inject your basal insulin at that time? Also, did you inject your breakfast bolus and any correction? How much bolus did you inject in total and can you explain how you came to that total? Was that reading whilst you were still in bed or had you got up and perhaps gone to the bathroom and maybe even having a coffee in the kitchen before you scanned? That is all really relevant information which will help you figure out what is going on.
Yes, I injected later than usual due to holidays. I took 14u of Levemir, cos thats what i am told, no maths required. Took 10u NR. 9u for 32g of carbs breakfast and 1 as correction dose. I used to follow 1:5 ratio but decided to be brave and lowered the ratio plus 1 extra unit. I usually sit up in bed and scan. Go to bathroom and inject. Prepare the breakfast and shower and then eat. It roughly takes 30mins.
What was your BG when you ate breakfast and how long did you wait?
I usually miss scanning at the time of eating.
It looks like your levels peaked in the 20s at 11.52am. Was there any particular reason why you scanned at that time? and did you take any action?
I usually scan around that time when i am about to go to the PG duty which is longer than an hour. No action taken.
Did you perhaps have a mid morning snack and possibly do a correction with it because your levels
no snack and no action taken.
have dropped a reasonable amount by just over an hour later when I am guessing you bolused for lunch and then they have continued to drop into the afternoon which might suggest that morning basal is too high or might be that you have stacked correctios or seriously miscalculated a bolus injection at lunch.
No idea what made it drop. Only bolused 5u for lunch. No corrections or stacking for that matter. Mind boggles.
Do you have any notes that you can explain what you ate and how much insulin you calculated for it and how much correction you took and if you had any snacks or did any corrections.
It must ve been a cheese sandwich with salad. None to the rest.
Having checked the next day's log, it shows the reverse pattern so you can't make any judgement on basal from those two days results ie no clear pattern, so skipping meals over a few days is going to be the only way to give you a clear picture.
That's what the real problem is. There aren't 2 days which are same. It confuses my already frazzled brain.
When you treat hypos, how disciplined are you?
if it is a real hypo. I treat it with 3 Lift glucose tabs. Scan again after 10 or so mins and usually i am on my way up. Lately the L2 has been showing false hypos. I always finger prick to double check.
On the 2nd of April, you scanned at 11.50 again and your levels were 9.9 and dropping rapidly (vertical downwards arrow) If that had been me, I would have scanned again in 10 mins and again in another 10 mins rather than wait until I was hypo and have to treat it. You can have a Jelly baby or a small amount of whatever you use to slow down a rapid drop like that if you get to 7 or 6 and it is still dropping to prevent yourself from having a hypo.
Thank you explaining with real numbers. 9.9 somehow means normal to me. I was told to eat something slow releasing if I am at 5 and am going to be out and about such as leaving work or going to PG duty.
When you treated the 3.8 hypo at 1355hrs, what did you have?
i was out. The GM read 4.2. I ate a medium banana to stop the downward trend. It must have been the late lunch which sent readings shooting upwards.
It would appear that you may have over treated it, since your levels bounced back up so high. I grade my hypo treatments according to how bad the hypo is. A 3.8 with a horizontal arrow would probably just get 1 or 2 jelly babies at most because it isn't significantly dropping any more and especially if it was just before I intended to have a meal as I want to keep my levels between 4 and 5 at the start of the meal, because it will only go upwards once I eat.
If I was 3.0 with a downward sloping arrow I would give it the full 3 jelly babies ie. 15g carbs. BUT my Libre alarm is set at 4.2 so when my alarm goes off, I have a jelly baby or two to prevent it going any lower.... again depending upon the arrow. If it was 4.2 with a vertical downward arrow, I might even have the full 3 JBs, definitely 2.
If there is one thing i am sure about re diabetes is not to over treat a hypo. If i am going low, i would take 1 gluco tablet. Check again. Still going down then i will take the other 2. Going low before pg duty or finishing work definitely demand a piece of fruit or a digestive. I am under the impression that after treating a hypo, must eat 10g of slow releasing carbs.
I almost never have slow acting carbs afterwards otherwise they will send my levels into orbit. I am very sensitive to carbs and my levels go up much easier than they come down so I have to be very stingy with my hypo treatment. Without knowing what you used for this hypo it is hard to tell if your liver kicked in and helped you out or if you too need to be mean with your hypo treatment OR perhaps you ate lunch straight after without bolusing for it.... or bolused after you had eaten lunch which would cause levels to go sky high again.
None of the above. No lunch straight after bolusing. No after the meal bolusing. Never.
Anyway, that is a very minor breakdown of some of the results over those two days, but without knowing exactly what you did when in detail, the amounts of insulin and the amounts af carbs and the timing of insulin and food and testing relative to getting put of bed etc, it is mostly speculation. I find looking at the graphs more helpful, but you still need to know all the background information for it to make sense like what your bolus was and how many carbs that was to cover and was there a correction involved and if so, how you come to that number of units. There is far too little data in what you have provided, but if you can answer all my questions above, I will look at it again.
Thank you for putting so much effort into my case scenario. I shall keep a detailed diary starting from tomorrow morning. Hoping for a positive outcome after all this hard work.
Thanking you again. Good night! Sleep well!!


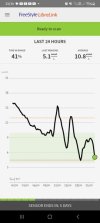
This last image is of today's graph.